 
Managed care organizations (MCOs) are groups, organizations, or other bodies that seek to reduce the cost of healthcare and increase the efficacy or health services through a number of means. Subscribers to indemnity plans have no restrictions on which providers they can see, but indemnity plans are typically much more expensive than managed care options, which we’ll review now. You’ll likely have a deductible and, depending on your insurance plan, a co-pay or co-insurance. Indemnity is the most basic and straightforward kind of insurance, in that you pay a premium to an insurance company to insulate you from medical expenses. Now that we’ve got an idea of how some of the basic aspects of health insurance work, let’s take a look at the different types of health insurance. The insurance company would pay the rest. For instance, if a subscriber receives a $300 medical procedure, and has a 80-20 co-insurance agreement with his or her insurance company, the subscriber would owe 20% of the bill ($60). Co-insurances are listed with the payer (insurance company)’s portion listed first, and then the subscriber’s. The co-pay does not count against the deductible.Ī co-insurance is a type of arrangement with the insurance company that divides the responsibility for payment by percentage. A copay is a relatively small, fixed sum that must be paid before any medical service is rendered. Subscribers may also have a copay or coinsurance arrangement with their insurance company. Many plans also have deductibles, which are monetary limits after which the health insurance company assumes the cost of the medical procedure or service. These may be assigned monthly or annually. 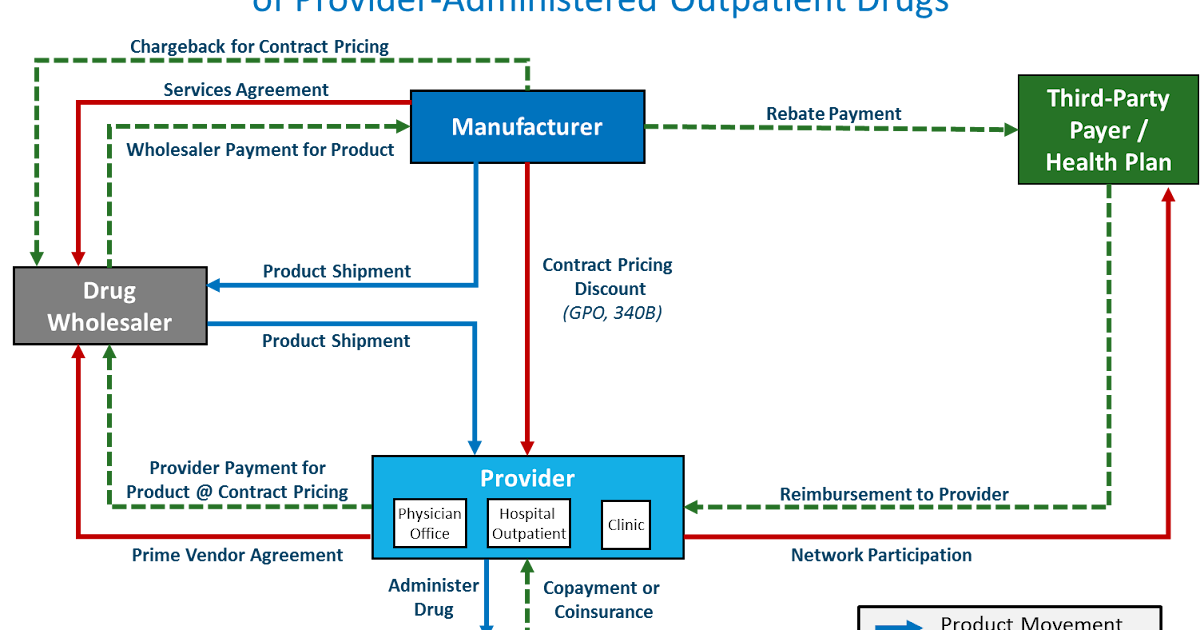
Most insurance plans require subscribers to pay premiums, which are essentially subscription fees. Most plans share a few basic similarities. 
There are many different types of insurance coverage plans, and even more ways of paying for them. How Health Insurance WorksĮssentially, health insurance subscribers enter into an arrangement with a health insurance company in order to reduce the impact of the cost of medical expenses. Americans spend almost $8,000 annually per capita on healthcare, and a significant portion of that sum is spent on health insurance. Manual check is done by our billers in order to ensure accuracy.Ī random quality audit, using statistical data.Healthcare is one of the largest and fastest-growing sectors of the American economy. Our Billers ensure layers of a quality Charge Entry Process in Medical Billing before submission of claims that ensures 100% clean claims submission the first time. CMS 1500 forms are also generated to submit to government agencies. Our Billers also submit claims to clearing houses to make sure that 100% accuracy is maintained for all our clients. Your fee schedule is taken into consideration and bills are raised accordingly. Every claim is verified to check: DOS, POS, Provider Info, Units, Modifiers, CPT code, Facility billed from, Referring Doctor in order to reduce the chance of claim rejection. Patient Demographics and Medical codes applied to charts are appropriately verified. It begins with filing claims for charge entry services provided to patients and creating bills, it’s all done electronically to shorten the revenue cycle days. Charge Entry Process in Medical Billing ServicesĬharge Entry Process in Medical Billing is the first step in the Medical billing process. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
